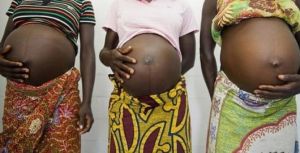
More than 50 per cent of expectant and new mothers experience perinatal depression, a situational analysis of mental health disorders related to pregnancy has shown.
Among the number, between 13 and 17 per cent develop suicidal intentions.
The analysis was conducted by the Ghana Health Service (GHS), in partnership with the Ministry of Health (MoH), the World Health Organisation (WHO), the UK-Foreign Commonwealth and Development Office (UK-FCDO), the Mental Health Authority, academia, Civil Society Organisations (CSOs) among other partners.
The report on maternal mental health was disseminated among key stakeholders in Accra last Tuesday.
Maternal mental health refers to the mental well-being of women during pregnancy, childbirth and the postpartum period and includes depression, anxiety, post-traumatic stress disorder and psychosis.
The exercise was to review literature, existing policies and the state of maternal mental healthcare to identify gaps, strengths and make recommendations that would improve mental health and mental healthcare delivery during and after pregnancy.
Stakeholders at the dissemination workshop included the WHO, the Ghana Medical Association, the Ghana Registered Nurses and Midwives Association, the Mental Health Authority, academia, scientists among others.
Gaps
Throwing more light on the report, a consultant to the WHO, Dr Promise Sefogah, said even though sufficient evidence existed on the adverse impact of maternal mental health disorders on mothers and infants, coupled with the high prevalence in the country, there was a little provision in the healthcare system for its screening, early detection and effective management.
He also mentioned the findings to include inadequate training of healthcare workers on maternal mental health and lack of knowledge on diagnostics, management and referral pathways.
He said the report, therefore, called for an integration of maternal mental health interventions within the health system along the entire value chain at all levels of care delivery and a national policy in that regard.
He also mentioned other recommendations to include high-level advocacy in Parliament, increased government investment in the sector and the inclusion of maternal mental health in the National Health Insurance policy to make it accessible and affordable for all.
The outgoing Minister of Health, Kwaku Agyeman-Manu, said maternal mental health issues could have significant implications for maternal and child health outcomes.
“Untreated maternal depression and anxiety can lead to adverse birth outcomes such as low birth weight and preterm birth and may affect breastfeeding practices and infant bonding.
“This can also lead to long-term consequences for emotional, cognitive and behavioural development of children,” he said.
“To address these challenges holistically and globally, WHO member states adopted and committed to meeting global targets of the Comprehensive Mental Health Action Plan 2013–2030 for improved mental health services to the people,” he explained.
Mr Agyeman-Manu said through the review, the government had made several efforts to ensure the provision of high-quality mental health services to the population.
He said strengthening the mental health system and ensuring that women had access to the support and care they needed during pregnancy and the postpartum period was a collective effort that required all levels of society to provide high-quality sustainable maternal mental health services.
“I wish to assure you that the Ministry of Health will provide the necessary leadership and direction to ensure the full implementation of the recommendations in this report,” he said.
WHO
In a speech read on his behalf, the Country Representative of WHO, Professor Francis Kasolo, said over the past decade, maternal health indices had been the priority of the global community with a focus on maternal mortality to the neglect of other conditions that affect the wellbeing of the mother, particularly her mental health.
Globally, evidence suggests that the prevalence of postpartum depression, anxiety and stress is relatively very high.
“The dissemination of the status report today is the first step in translating policy into action and I want to congratulate the Ministry of Health, the Ghana Health Service, the Mental Health Authority, academia and civil society organisations on your commitment in conducting this assessment.
“The WHO and partners would continue to work with the Ministry of Health and its agencies to ensure that identified strengths and opportunities such as the Network of Practice (NoP) approach are leveraged in developing specific interventions that promote the integration of maternal mental health services into routine perinatal care across various levels of service delivery,” he said.
He said that would ensure improvement in the well-being of pregnant and postpartum women generally, as well as focused intervention targeting those with vulnerabilities such as adolescent girls, women with disabilities and those who have suffered foetal loss.
Neglect
In a speech read on his behalf, the Director-General of the Ghana Health Service, Dr Patrick Kuma-Aboagye, said it was an undeniable fact that the bid to significantly reduce preventable maternal and newborn mortality had diverted attention from the agony and personal sad stories of numerous women and families that go unnoticed even in health facilities.
He said improving the quality of maternal and newborn care as outlined in the Reproductive Maternal, Newborn, Child and Adolescent Health (RMNCAH) strategic plan 2020-2025 would require considerable improvement in the individual experience of women during childbirth, with particular attention to their psychological and social wellbeing.
“It is worth noting that in childbirth in its entirety, the related vulnerabilities place a mental health burden on women, if not supported.
The situational analysis has provided significant insights into the structure gaps in our healthcare setting, the extent of the human resource challenges in mental health and the highly stigmatising environment we live, in our communities.
“Nevertheless, these are the opportunities to craft pathways for more humane and enabling care through promoting family involvement and support during childbirth, which has traditionally characterised our society.
“Improving access to maternal mental health services in a congenial atmosphere, supported by the right skills mix and equitable distribution of healthcare workers with the capacity to deliver comprehensive and integrated maternal mental health services at all levels of care, needs to be prioritised,” he said.
Source: graphiconline
| Disclaimer: Opinions expressed here are those of the writers and do not reflect those of Peacefmonline.com. Peacefmonline.com accepts no responsibility legal or otherwise for their accuracy of content. Please report any inappropriate content to us, and we will evaluate it as a matter of priority. |
Featured Video